In Vitro Fertilization (IVF) in Thailand
Search and Compare the Best Clinics and Doctors at the Lowest Prices for In Vitro Fertilization (IVF) in Thailand






In Vitro Fertilization (IVF) at Sikarin Hospital in Bangkok, Thailand





In Vitro Fertilization (IVF) at Bangkok Hospital Phuket in Phuket, Thailand





In Vitro Fertilization (IVF) at Thonburi Bamrungmuang Hospital in Bangkok, Thailand





In Vitro Fertilization (IVF) at Bangkok Hospital Bangkok in Bangkok, Thailand





In Vitro Fertilization (IVF) at Genea IVF and Genetics in Bangkok, Thailand





In Vitro Fertilization (IVF) at Bumrungrad International Hospital in Bangkok, Thailand
Our partner clinics in are accredited by the following associations












































































































































No Time?
Tell us what you're looking for and we'll reach out to the top clinics all at once
WHY US?












































































































































No Time?
Tell us what you're looking for and we'll reach out to the top clinics all at once
What does a In Vitro Fertilization (IVF) Procedure Involve?
IVF is a long process and may take several months to be complete. Although this procedure will increase your chances of getting pregnant, there’s still no guarantee that it will all be effective to all.
Before performing IVF procedures, you and your partner must first undergo a series of tests such as Semen analysis, Ovarian reserve testing, Infectious disease screening, Mock embryo transfer, and Uterine cavity exam.
After the screening, both of you will now undergo IVF procedures:
- Fertility medications - these are prescribed medications to stimulate your ovaries to increase your egg production. Multiple eggs must be produced because it is expected that some eggs will not develop or be fertilized after retrieval. During this stage, a transvaginal ultrasound is used to check the ovaries and also a blood test will be administered to check your hormone levels. Your eggs will be collected through minor surgery. This procedure will be done by using the latest ultrasound technology to guide a needle in each of your ovaries for egg extraction. Usually, propofol-based anesthesia will be used while you undergo the procedure.
- Sperm sample - Your partner will now be asked to produce a sperm sample that will be combined with your extracted eggs for fertilization. If you will be using donated sperm, it will be removed from being frozen and will be prepared the same way.
- Insemination - In this procedure, the eggs and sperm will be mixed together and be stored in a laboratory dish to undergo fertilization. If in case there is a low possibility of fertilization, intracytoplasmic sperm injection (ICSI) may be used. By doing this, a single sperm will be directly injected into the egg; the eggs will be closely monitored if fertilization will occur.
- Embryo Transfer- Once fertilization is successful, cell division will take place; fertilized eggs are now called embryos. These embryos will now be transferred to your uterus 3-5 days upon egg retrieval and fertilization. For women under 40, one or two embryos can be transferred and for women aged 40 and above, a maximum of 3 embryos can be transferred. The number of embryos to be transferred must be restricted to prevent the risks of multiple births.
How Long Should I Stay in Thailand for a In Vitro Fertilization (IVF) Procedure?
Although it is advisable that you will need to take it easy after the embryo transfer, some women are able to resume their normal daily routine after the procedure. Note that your scheduled follow-up checkups with your surgeon are essential to your recovery and healing and you will be expected to stay in Thailand for 10-12 days. However, you must also be aware of its possible side effects:
- Passing a small amount of fluid (may be clear or blood-tinged) after the procedure
- Mild cramping and/or bloating
- Constipation
- Breast Tenderness
What's the Recovery Time for In Vitro Fertilization (IVF) Procedures?
Although the In Vitro Fertilization (IVF) isn't a surgery procedure, it consists of specific methods that call for a recuperation period. After the embryo has been inserted, it's common for medical professionals to advise a brief rest interval. The human body requires a span of adjustment in anticipation of possible conception, hence the importance of granting it the needed time.
The actual recovery from the specific stages of the embryo implantation and egg collection is typically rapid, generally inside a day or possibly two. However, the actual recuperation and waiting period expands to roughly a fourteen-day period following the embryo insertion - infamously known as the "two-week wait". This timeframe marks the potential start ofearly pregnancy stages, and can serve as both a physical and emotional healing process from the procedure.
The hormone-based medications administered as part of the In Vitro Fertilization (IVF) can also bring about symptoms such as fluid retention, stomach ache, mood fluctuations, and sensitivity where the injection is administered. These symptoms are apt to decrease as your body accustoms to the hormonal variation, but they could add to the duration of the recovery phase.
What sort of Aftercare is Required for In Vitro Fertilization (IVF) Procedures?
Following your In Vitro Fertilization (IVF) process, ensuring strict adherence to post-procedure instructions becomes a crucial part of your recovery journey. This could encompass a variety of elements such as medicinal, dietary, physical, and mental health-based measures. Hormonal injections could continue for a few days or weeks post the embryo transplantation.
Furthermore, many clinics offer explicit dietary plans that you are expected to adhere to. This involves a significant shift toward consuming more nourishing food, increasing your water intake, and refraining from certain dietary habits. Your diet significantly influences the embryo's growth by setting up ideal conditions. It's important to note that your well being should never be neglected. Adequate rest, efficient stress management, and abstaining from strenuous exercises are suggested to maintain your health at an optimal level for successful conception.
Post-procedure care typically provided by the clinic includes regular monitoring of your hormonal levels and general health. You may experience slight discomforts such as mild bloating, and constipation following the procedure, for which the medical team will provide relevant advice and medical attention. A pregnancy test is slated for about a fortnight following the embryo transplantation. Provided the test is positive, your clinic will either transition your care to your usual OB/GYN or handle your prenatal care management as needed.
Moreover, counseling is very important when you are having IVF; everyone must fully understand that not all IVF procedures have successful outcomes. It is highly recommended that couples should have proper counseling during and after IVF treatment
What's the Success Rate of In Vitro Fertilization (IVF) Procedures?
Assessing the effectiveness of the In Vitro Fertilization (IVF) requires a comprehensive analysis. The effectuality rates can be substantially impacted by various elements, such as the patient's age and overall wellness, the reason behind infertility, the specific procedure implemented, and lifestyle elements like dietary habits and physical activity routines. 40% of Women under the age of 35 will be successful and 25% of women aged 36 to 41 will be successful and only 4% over the age of 42 will be successful. You must also understand that pregnancy rates are not exactly the same as the live birth rate.
Moreover, the aptitude and proficiency of the involved healthcare experts should also be factored in. For example, the patient's age is a vital factor in determining success rates, with younger women generally having healthier egg cells, thereby elevating the possibility of IVF success. Essentially, the capabilities of the clinic, the technology within the lab, and the embryologist's professional expertise collectively contribute to the outcome of the procedure. Therefore, taking these aspects into account, it becomes crucial to opt for a clinic recognized for its high success rates.
Are there Alternatives to In Vitro Fertilization (IVF) Procedures?
In Vitro Fertilization is not the only possible treatment for infertility. Other fertility treatments to consider may include:
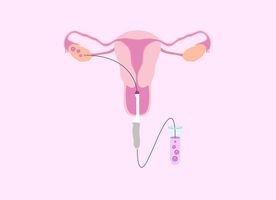
- Intrauterine Insemination - commonly known as artificial insemination. In this procedure, sperm is inserted via the cervix into your uterus when you’re ovulating.
- Surgery - in some cases both males and females must undergo a corrective surgical procedure if their reproductive organs are the ones causing fertility issues. Such corrective surgical options can help without the need for other infertility treatments.
- Lifestyle changes - instead of undergoing any infertility treatment, your fertility specialist may suggest that you make a series of lifestyle changes that may be causing such problems. This may involve weight reduction, reducing alcohol consumption, and quitting smoking.
This information has been accurately sourced and verified by a medical professional for its accuracy, however, we strongly recommend you to consult with your doctor before pursuing medical procedures overseas.