Gynecologic Laparoscopy in Romania
Find the best clinics for Gynecologic Laparoscopy in Romania
No pricing info available
United States offers the best prices Worldwide
Price: $ 60
From 18 verified reviews
Mariana Iliescu, 21 January 2020
Great team. Good services.
From 8 verified reviews
Nico, 17 September 2020
Nu vom uita niciodata numele Dnei Dr Codreanu Dorina. Ii datoram recunostina pentru cele doua minuni pe care le avem acasa. Fara dansa nu am fi fost niciodata parinti. Un medic exceptional, empatica, foarte bine pregatita...un profesionist! Jos palaria pentru Doamna Dr!
WHY US?
At Medijump, we're making medical easy. You can search, compare, discuss, and book your medical all in one place. We open the door to the best medical providers worldwide, saving you time and energy along the way, and it's all for FREE, no hidden fees, and no price markups guaranteed. So what are you waiting for?

Free

Best Price

Widest Selection

Risk-Free
What you need to know about Gynecologic Laparoscopy in Romania
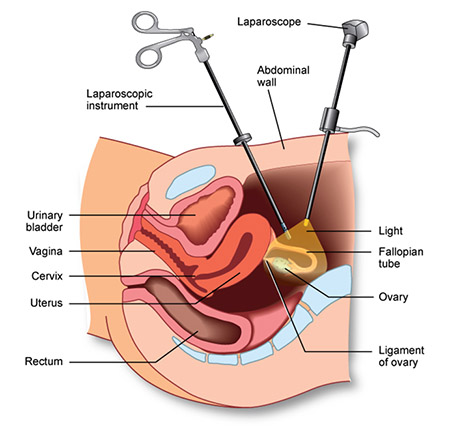
Gynecologic laparoscopy is a procedure in which a surgeon uses a laparoscope (a long, thin tube with a high-resolution camera and a high-intensity light at its end) to see inside your lower abdomen. The camera on the laparoscope sends images to a video monitor. This means that the surgeon will be able to see your ovaries, fallopian tube, and uterus (womb) in real-time, without open surgery. They will also be able to see other parts of the body, such as the bowel and bladder.
Gynecologic laparoscopy can be used to determine what’s causing your symptoms, as well as treating various conditions. It can be done to:
-
Diagnose and treat endometriosis (endometrial tissue ablation)
-
Diagnose and remove an ovarian cyst
-
Diagnose infertility
-
Diagnose pelvic abscess or pus
-
Diagnose pelvic inflammatory disease
-
Diagnose and treat fibroids
-
Diagnose and treat an ectopic pregnancy (a condition in which a fertilized egg starts to develop outside of your womb)
-
Remove scar tissue (scars can develop after infections, such as pelvic inflammatory disease or endometriosis)
-
Perform tubal ligation or sterilization (cutting or closing your fallopian tubes to permanently prevent pregnancy)
-
Remove your ovaries (oophorectomy) or womb (hysterectomy)
-
Diagnose cancer or investigate whether cancer has spread.
During a gynecologic laparoscopy, the surgeon may take a small sample of tissue (biopsy). This sample can be sent to a laboratory for testing to see whether the cells in the sample are cancerous or not cancerous.
What does the Procedure Involve?
Gynecologic laparoscopy is usually performed under general anaesthesia. Once your surgeon gives you the anaesthetic, a small tube called a catheter will be used to collect your urine. Then, your surgeon will use a small needle to fill your abdomen with carbon dioxide gas. The gas is needed to reduce the risk of injury by keeping your abdominal wall away from your organs.
A small cut in your abdomen near the belly button will be made to insert the laparoscope, which conveys images to a monitor screen. The images give your surgeon a clear, real-time view of your organs. What happens after depends on why a gynecologic laparoscopy is performed.
-
For diagnosis purposes, your surgeon might take a look and try to find any abnormality.
-
For treatment purposes, your surgeon will make other incisions to insert tiny surgical instruments. Then, the treatment is performed using the laparoscope as a guide.
When the procedure is over, your surgeon will remove all instruments and close the incisions with stitches.
How Long Should I Stay in Romania?
If you are having a gynecologic laparoscopy to diagnose a condition, you should be able to leave the hospital on the same day. If you have the procedure to treat a condition, you may need to stay in the hospital overnight. In general, it is recommended that you stay in Romania for 5 to 7 days following your gynecologic laparoscopy as you need to let your body recover first and attend follow-up checkups.
What's the Recovery Time?
Recovery time for gynecologic laparoscopy varies, depending on what procedure was performed. You may need to rest for a week. After diagnostic gynecologic laparoscopy, you may be able to resume all normal activities in one or two weeks. However, if the procedure is done to treat a condition, it may take 4 weeks or more until you can return to normal activities.
What About Aftercare?
Your medical team will give you instructions on how to care for yourself at home before you are discharged from the hospital. In general, you need to keep the following instructions in mind:
-
Your doctor may prescribe pain medication to ease your discomfort or antibiotics to prevent an infection. Make sure to take the medications as prescribed.
-
Rest and get enough sleep to help you recover. However, try to walk every day to boost blood flow.
-
Drink plenty of fluids.
-
If your doctor allows you, you may shower within one or two days following the surgery. However, don’t take a bath until your doctor says it’s okay.
-
Always attend the scheduled follow-up checkups.
What's the Success Rate?
Gynecologic laparoscopy is a safe procedure. It is a highly successful procedure that allows your surgeon to easily diagnose any problems and treat various conditions without having to open your lower abdomen. However, there are still some side effects and risks you need to be aware of. These include bleeding from your vagina, pain in your abdomen, nausea, tiredness, and shoulder pain, development of a blood clot, infection, and damage to other organs.
Are there Alternatives to Gynecologic Laparoscopy?
For diagnostic purposes, you can consider an ultrasound scan or MRI scan instead of a gynecology laparoscopy. Both of these procedures are non-invasive. For treatment purposes, laparotomy or open surgery can be an alternative. This involves making a large cut in your abdomen. It is usually used for bigger operations, such as a hysterectomy.
What Should You Expect Before and After the Procedure
Before gynecologic laparoscopy, you may experience unexplained pelvic pain or unexplained infertility, or you may have a condition in your reproductive system that needs to be treated. After the procedure, the cause of your symptoms or infertility will be shown and your doctor can create a treatment plan. Any condition you have before the procedure will be treated.
Whilst the information presented here has been accurately sourced and verified by a medical professional for its accuracy, it is still advised to consult with your doctor before pursuing a medical treatment at one of the listed medical providers
No Time?
Tell us what you're looking for and we'll reachout to the top clinics all at once
Enquire Now

Popular Procedures in Romania
Prices Start From $17

Prices Start From $714

Prices Start From $69

Recommended Medical Centers in Romania for Gynecologic Laparoscopy

- Interpreter services
- Translation service
- Religious facilities
- Medical records transfer
- Medical travel insurance
- Health insurance coordination
- TV in the room
- Safe in the room
- Phone in the room
- Private rooms for patients available

- Interpreter services
- Translation service
- Religious facilities
- Medical records transfer
- Medical travel insurance
- Health insurance coordination
- TV in the room
- Safe in the room
- Phone in the room
- Private rooms for patients available

- Interpreter services
- Translation service
- Religious facilities
- Medical records transfer
- Medical travel insurance
- Health insurance coordination
- TV in the room
- Safe in the room
- Phone in the room
- Private rooms for patients available

- Interpreter services
- Translation service
- Religious facilities
- Medical records transfer
- Medical travel insurance
- Health insurance coordination
- TV in the room
- Safe in the room
- Phone in the room
- Private rooms for patients available


